Oct. 25, 2013 Press Release Biology Medicine / Disease
Hope of new treatment for severe asthma patients
New research from Japan brings hope of a new treatment for asthma patients resistant to corticosteroids. In a study published today in the journal Nature Communications, researchers from the RIKEN Center for Integrative Medical Sciences and Keio University in Japan report that a type of lymphocytes called natural helper (NH) cells plays a critical role in corticosteroid resistance and demonstrate that the anti-psychotic drug Pimozide can be used to overcome resistance to steroids in severe asthma patients.
Asthma is a chronic disease characterized by a persistent inflammation of the airways. The condition can be controlled with a moderate dose of inhaled corticosteroids in most patients. However, 5-10% of patients with “severe asthma” respond poorly to a maximal dose of steroids. These patients experience uncontrolled and frequent asthma symptoms that have a profound impact on their quality of life and health care costs. Unveiling the mechanism leading to steroid resistance in these patients is therefore crucial for the development of a new, effective therapy.
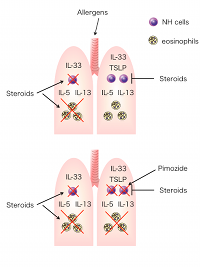
T lymphocytes and NH cells in the asthmatic lung produce proteins named interleukin (IL)-5 and IL-13 that are responsible for severe airway inflammation. In asthma patients, inhaled steroids function by suppressing both T lymphocytes and NH cells.
However, in severe asthma patients, another protein called interleukin-33 (IL-33) produced in the airways strongly activates NH cells to produce IL-5 and IL-13, leading to severe airway inflammation.
In the current study, the researchers led by Drs Shigeo Koyasu from RIKEN and Koichiro Asano from Keio University, employed an experimental mouse model for airway inflammation to study the pathway leading to IL-33-mediated NH activation. Their research shows that NH resistance to steroids is induced by the protein thymic stromal lymphopoietin (TSLP), present in the airways of severe asthma patients.
The team tested reagents that block the intracellular signals triggered by TSLP in NH cells. They identified one drug, Pimozide, an approved anti-psychotic drug, that restored the effects of steroids on NH cells.
“Therefore, administration of Pimozide or related drugs would be an effective treatment in human severe asthmatic patients,” conclude the authors.
Reference
- Kabata, H. Moro, K. Fukunaga, K. Suzuki, Y. Miyata, J. Masaki, K. Betsuyaku, T. Koyasu, S. and Asano K. Thymic stromal lymphopoietin induces corticosteroid resistance in natural helper cells during airway inflammation. Nature Communications, 2013, doi: 10.1038/ncomms3675.
Contact
Shigeo Koyasu, Group Director
Laboratory for Immune Cell System
RIKEN Center for Integrative Medical Sciences
Jens Wilkinson
RIKEN Global Relations and Research Coordination Office
Tel: +81-(0)48-462-1225 / Fax: +81-(0)48-463-3687
Email: pr@riken.jp
