Jul. 10, 2009 Research Highlight Biology
Natural suppressors of a treatment-induced disease
A naturally occurring population of dendritic cells reduces the incidence and severity of graft-versus-host-disease in mice
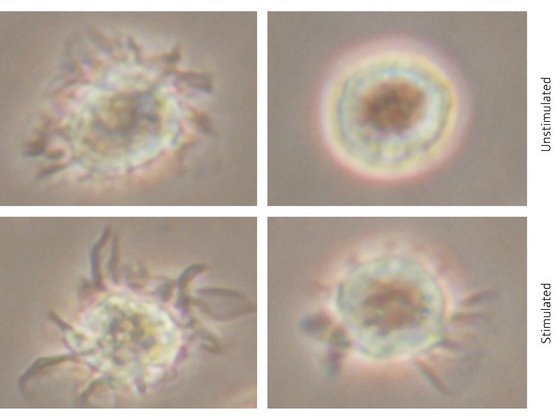 Figure 1: Phase contrast microscopy images (original magnification × 400) showing the morphology of non-regulatory (CD11c+) DCs (left column) and CD200R3+ DCregs (right column) before and after stimulation with a pro-inflammatory agent.
Figure 1: Phase contrast microscopy images (original magnification × 400) showing the morphology of non-regulatory (CD11c+) DCs (left column) and CD200R3+ DCregs (right column) before and after stimulation with a pro-inflammatory agent.
Researchers in Japan have shown that mouse dendritic cells (DCs), which can promote or inhibit inflammation depending on the proteins displayed on their surface, include a subpopulation that exerts beneficial effects during a treatment for leukemia and other malignancies. The treatment—known as allogeneic hematopoietic stem cell transplantation (alloHSCT)—can, in some situations, result in graft-versus-host-disease (GVHD). Acute and chronic GVHD occur when donor immune cells called T lymphocytes recognize and become activated by proteins present on recipient but not donor tissues. The resulting T lymphocyte-driven immune response can result in severe damage to the recipient skin, gastrointestinal tract and liver.
Previous work by these researchers described the generation of regulatory DCs from mouse bone marrow (BM-DCregs) that, when injected after alloHSCT, reduce the severity and incidence of acute and chronic GVHD. The team, led by Katsuaki Sato at the RIKEN Research Center for Allergy and Immunology in Yokohama, has now shown that naturally occurring counterparts of BM-DCregs exist and influence the outcome of alloHSCT in mice1.
The researchers started by searching for genes associated with immunosuppressive DC function. A comparison of the genes expressed in BM-DCregs and non-regulatory DCs revealed that the gene encoding the surface protein CD200R3 is expressed exclusively in BM-DCregs. They found that blockade of CD200R3 impaired the ability of BM-DCregs to suppress proliferation of T lymphocytes, whereas forced expression of CD200R3 in non-regulatory DCs reduced their ability to promote T lymphocyte cell division. This indicates that CD200R3 contributes to the immunosuppressive function of BM-DCregs.
Reasoning that naturally occurring regulatory DCs might also express CD200R3, the researchers screened blood and spleen cells for CD200R3 expression. They identified a small population of CD200R3-expressing cells that, like BM-DCregs, produced immunosuppressive cytokines, which are regulators of the immune system, and inhibit T cell proliferation. These CD200R3+ DCs exhibited a different morphology than non-regulatory DCs (Fig. 1).
When injected after alloHSCT, Sato and colleagues found that these CD200R3+ DCs—like BM-DCregs—suppressed the onset and severity of GVHD. Recipients of CD200R3+ DCs contained lower amounts of serum proinflammatory proteins, and higher numbers of immunosuppressive regulatory T lymphocytes. Further highlighting the biological importance of CD200R3+ DCs, pre-treatment with a CD200R3-blocking antibody prior to alloHSCT exacerbated GVHD.
“The functional identification of naturally occurring human DCregs, as well as their counterparts generated the laboratory, may provide an advantageous means of intervening to prevent chronic GVHD after alloHSCT” says Sato.
References
- 1. Sato, K., Eizumi, K., Fukaya, T., Fujita, S., Sato, Y., Takagi, H., Yamamoto, M., Yamashita, N., Hijikata, A., Kitamura, H., Ohara, O., Yamasaki, S., Saito, T. & Sato, K. Naturally occurring regulatory dendritic cells regulate murine cutaneous chronic graft-versus-host disease. Blood 113, 4780–4789 (2009). doi: 10.1182/blood-2008-10-183145
