Nov. 2, 2016 Press Release Biology Medicine / Disease
New iPS-cell model system helps develop treatments for spinocerebellar ataxia
Researchers at the RIKEN Center for Developmental Biology have succeeded in creating a new model system that can be used to develop drug therapies for genetic disorders like spinocerebellar ataxia type 6 (SCA6). Published in Cell Reports, the study shows how stem cells from patients with SCA6 can be transformed into mature Purkinje cells — the same type of neuron that starts dying when people develop SCA6 later in life. With this setup, the team discovered that mature Purkinje cells with the SCA6 mutation became vulnerable when deprived of thyroid hormone.
SCA6 is a movement disorder characterized by death of Purkinje cells in the cerebellum, a brain region that controls our ability to produce smooth movements. No effective treatment or cure exists for this neurodegenerative disorder, and animal models have proved inconclusive. As an alternative, the team led by Keiko Muguruma focused their efforts on making a disease model based on human Purkinje cells grown in culture.
As Muguruma explains, “we succeeded in generating Purkinje cells with full sets of SCA6 patient genes. Unlike animal models, these patient-derived Purkinje cells will be extremely useful for investigating disease mechanisms and for developing effective drug therapies.”
The disease manifests in middle age and results from mutations that increase the number of times a particular section of the CACNA1A gene are repeated. The researchers first induced skin or blood cells from patients and control participants to become pluripotent stem cells. Then they used techniques recently developed in their lab to create self-organizing cerebellar tissue and Purkinje cells.
When tested, the team found that while both types of mature Purkinje cells seemed outwardly similar, they differed in how much the CACNA1A gene was expressed. The patient-derived cells contained more of the protein encoded by the CACNA1A gene than the normal cells. When immature cells were tested, protein expression levels were similar, regardless of their origins.
The part of the CACNA1A protein that contains the excessively repeated section is called α1ACT. When researchers compared expression of this fragment between normal and patient-derived cells, they found that it was expressed much less in the SCA6 Purkinje cells. Because α1ACT normally binds to DNA in the nucleus and triggers the expression of other proteins that are important for normal Purkinje-cell development, these proteins were also expressed much less in the cells that contained the mutation. Again, when the team looked at immature Purkinje cells, α1ACT expression was similar for all groups.
“This new system is particularly useful for drug discovery,” notes Muguruma. “Using it, we were able to demonstrate that patient-derived Purkinje cells show a vulnerability to nutrient depletion and that this vulnerability can be suppressed by several compounds.”
Knowing that thyroid hormone is important for proper maturation and maintenance of Purkinje cells, the researchers deprived mature neurons of the hormone and found that many of the patient-derived cells died, while those that survived showed physical abnormalities. Purkinje cells without the mutation were unaffected. Further testing showed that even when deprived of thyroid hormone, negative changes in SCA6 Purkinje cells could be prevented using thyroid releasing hormone. Similar results occurred with Riluzole, a drug often used to treat another neuromuscular disorder called ALS — also known as Lou Gehrig's disease.
Decreased thyroid gland activity, a condition known as hypothyroidism, also occurs with age, and might be linked to SCA6 onset. Muguruma cautions, “there are some reports that hypothyroidism is related to cerebellar ataxia and cerebellar atrophy, but we do not yet know whether the SCA6 disease phenotypes are causally linked to decreased thyroid hormone.”
Now that they have proved the usefulness of this model system, Muguruma and her colleagues can continue to investigate how thyroid releasing hormone was able to protect the cells, and ultimately find a cure for this type of spinocerebellar ataxia.
Reference
- Yoshihito Ishida, Hideshi Kawakami, Hiroyuki Kitajima, Ayaka Nishiyama, Yoshiki Sasai, Haruhisa Inoue, and Keiko Muguruma, "Vulnerability of Purkinje cells generated from spinocerebellar ataxia type 6 patient-derived iPS cells", Cell Reports, doi: 10.1016/j.celrep.2016.10.026
Contact
Research Specialist
Keiko Muguruma
Laboratory for Cell Asymmetry
RIKEN Center for Developmental Biology
Adam Phillips
RIKEN International Affairs Division
Tel: +81-(0)48-462-1225 / Fax: +81-(0)48-463-3687
Email: pr@riken.jp
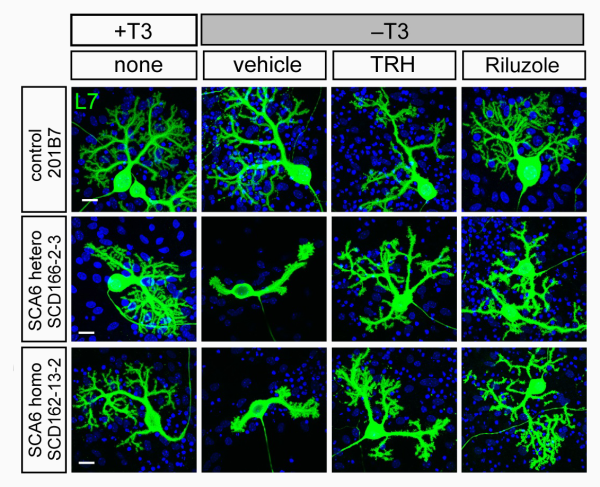
T3-depletion induced damage to SCA6 Purkinje cells is suppressed by drug treatments
High magnification images of L7+ Purkinje cells (green) derived from control (top), SCA6 heterozygous (middle) and SCA6 homozygous (bottom) iPSCs on culture day 75. Note the dendritic degradation when SCA6 cells are deprived of thyroid hormone T3, and the lack of degradation when thyroid releasing hormone (THR) or Riluzole are present. Scale bars, 200 μm.
